
Digestive Health
By Dr Saravana.K
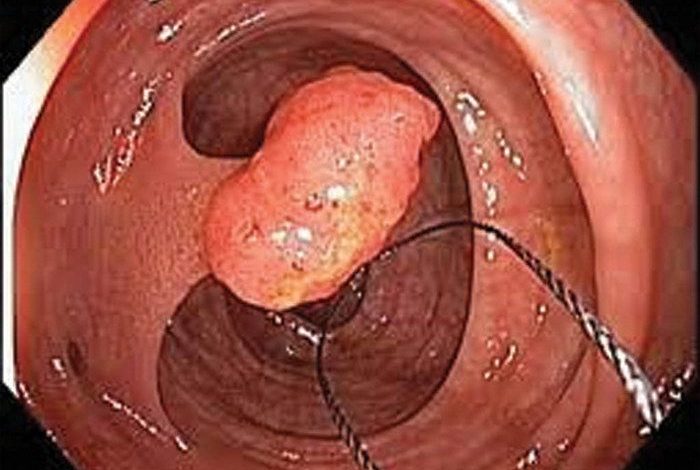
Colonic polyp is a small clump of cells that forms on the lining of the colon. Most polyps are harmless but over time, some can develop into colon cancer, which is often fatal when found in its later stages.
Anyone can develop colon polyps. You’re at higher risk if:
- Age. Most people with colon polyps are 50 or older.
- Inflammatory intestinal conditions, such as ulcerative colitis and Crohn’s disease.
- Family history. You’re more likely to develop colon polyps or cancer if you have a parent, sibling or child with them. If many family members have them, your risk is even greater. In some people, this connection isn’t hereditary.
- Tobacco and alcohol use.
- Obesity and lack of exercise.
It’s important to have regular screening tests, such as colonoscopy, because polyps found in the early stages can usually be removed safely and completely. The earlier polyps are removed, the less likely it is that they will become malignant.
You should be screened regularly for polyps if:
- You’re age 50 or older.
- You have risk factors, such as a family history of colon cancer. Some high-risk individuals should begin regular screening much earlier than age 50.
The best prevention for colon cancer is regular screening for polyps. Screening methods include:
Colonoscopy, the most sensitive test for colorectal polyps and cancer. If polyps are found, your doctor may remove them immediately or take tissue samples (biopsies) for analysis. It’s important to fully prepare your colon before colonoscopy. If stool remains in the colon and obstructs your doctor’s view of the colon wall, you will likely need a follow-up colonoscopy sooner than the guidelines specify.
Your doctor is likely to remove all polyps discovered during a bowel examination. The options for removal include:
- Removal during screening. Most polyps can be removed with biopsy forceps or a wire loop that snares the polyp. This may be aided by injecting a liquid under a polyp to lift it off the wall for removal.
- Minimally invasive surgery. Polyps that are too large or that can’t be reached safely during screening are usually removed using minimally invasive surgery.






A doctor who specializes in analyzing tissue samples (pathologist) usually must examine polyp tissue under a microscope to determine whether it’s potentially cancerous. If you have had an adenomatous polyp or a serrated polyp, you are at increased risk of colon cancer. You’ll need follow-up screenings colonoscopy for polyps and the time interval would depend on the tissue type, size and number of polyps which were removed.
Colon polyps often cause no symptoms. You might not know you have a polyp until your doctor finds it during an examination of your bowel.
But some people with colon polyps experience: rectal bleeding; change in stool colour; change in bowel habits; pain, nausea or vomiting; or iron deficiency anemia.
Prevention
You can greatly reduce your risk of colon polyps and colorectal cancer by having regular screenings. Certain lifestyle changes also can help: eat fruits, vegetables and whole grains; reduce your fat intake; limit alcohol consumption; don’t use tobacco; and stay physically active and maintain a healthy body weight.


