
Digestive Health
By Dr Saravana.K
The esophagus is the muscular tube that extends from the neck to the abdomen and connects the throat to the stomach. Achalasia is a condition where the esophagus is unable to move food into the stomach. The lower esophageal sphincter (LES), a valve located at the end of the esophagus, stays closed during swallowing, resulting in the back up of food.


Difficulty swallowing, regurgitation of undigested bitter food, chest pain and heartburn.
Who is affected by achalasia?
It is typically diagnosed in adults, but can occur in children as well. There is no particular race or ethnic group that is affected, and the condition does not run in families.
Is achalasia serious?
As the condition advances, achalasia can cause considerable weight loss and malnutrition. People with achalasia also have a small increase in the risk of developing esophageal cancer, particularly if the obstruction has been present for a long time.
How is achalasia diagnosed?
- Barium swallow. The patient swallows a barium preparation (liquid form) and its movement through the esophagus is evaluated using X-ray.
- Endoscopy. A flexible, narrow tube called an endoscope is passed into the esophagus and projects images of the inside of the esophagus onto a screen.
- Manometry. This test measures the timing and strength of esophageal (pump) contractions and LES relaxation.


If left untreated, achalasia can be debilitating. People with the condition experience considerable weight loss that can result in malnutrition. Lung infections and pneumonia due to aspiration of food can result, particularly in the elderly. There are several successful treatments available for achalasia, including:
Minimally Invasive Surgery
Today, select patients with achalasia can be treated successfully by a minimally invasive surgical technique called laparoscopic esophagomyotomy where the muscles of the valve between the esophagus into the stomach are cut. This operation usually requires one day of hospital stay and recovery is typically accelerated when compared to conventional surgery. Up to two-thirds of patients are treated successfully with surgery, though some patients may have to repeat the surgery or undergo balloon dilation to achieve satisfactory long-term results.
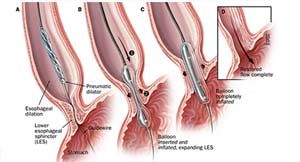
Balloon Dilation
While the patient is under light sedation, the gastroenterologist inserts a specially designed balloon through the LES and inflates it. The balloon disrupts the esophageal muscle and widens the opening for food to enter the stomach. Some patients may have to undergo repeated dilation treatments in order to achieve symptom improvement.
On average, this procedure offers a 75 per cent chance of relieving symptoms for a period of years. Risk associated with the procedure, however, is potential perforation of the esophagus.
Medication
Patients who are not appropriate candidates for balloon dilation or surgery may benefit from Botox® (botulinum toxin) injections. When injected into muscles in very small quantities, Botox can relax spastic muscles.


